Month: May 2020

Getting your child a speech generating device (SGD) is an exciting step towards improving their communication and independence. It’s an exciting time, but it is not a quick fix and doesn’t mean that your child can immediately begin to communicate with you. A baby is consistently hearing verbal communication every day for a year or more before they begin using words and phrases to communicate, and the same goes for a child being introduced to a speech generating device (SGD). This is done in many places- therapy, school, the community, and most importantly, HOME! Language learning does not stop when your child walks in the door from a long day of school or therapy, and their SGD needs to be introduced and modeled by other people at home when communicating with the child. Here are some tips to help you incorporate your child’s speech generating device into your daily routine at home-
– Learn about your child’s device. Know where the vocabulary “buttons” are, how to navigate across the pages, and how to customize it to your child. Don’t be afraid to ask your therapist for help during this time, they are a great resource!
– Have their device present at all times. Think of the SGD as their voice, and remember to take it anywhere you would expect your child to talk with you while playing, eating, cleaning, or even doing homework.
– Model for the child on their device, and don’t be afraid to use the SGD yourself when communicating with them! Show your child how to activate the “buttons” of one or more vocabulary words from the phrase you’re saying verbally. This video can help you better understand this idea!
– Try to stay a step ahead of your child. A child doesn’t wake up using verbal phrases, and they aren’t going to do this with a device either. When modeling, try to show your child phrases that are a step longer than what they typically produce- if they are using a single word or button activation on the SGD to communicate, try to model two to three-word phrases on their device so that they are consistently seeing and hearing gradual expansions of their productions.
– Help the child use their device outside of the home as well. Places like the park, grocery store, and restaurants have many opportunities to model new vocabulary and encourage requesting from your child!
It’s important to consistently reinforce what your child is learning at therapy and school at home so that they are generalizing their skills to new environments, and home practice can make a big difference in a child’s ability to communicate in a variety of places.
If you have any questions about the use of speech generating devices or how to better help your child with their device, reach out to us at http://www.abcpediatrictherapy.com. We are here to educate you and inspire your child.
Kiddos who are chronic toe walkers or have increased muscle tone in their calf muscles lack the range of motion in their ankles to be able to walk with a normal heel-to-toe pattern. It also affects their balance and can cause muscular imbalances throughout the body due to using incorrect muscles to compensate. This then leads to difficulty performing and attaining new gross motor skills, leaving them behind compared to their peers.
In mild cases, this muscle tightness can be helped with a course of physical therapy and a home exercise program consisting of activities such as stretching, strengthening exercises, and gait training (activities to work on walking heel-to-toe). In more severe cases, however, physical therapy alone is limited. Research has proven that kiddos lacking a significant amount of range of motion benefit from something called serial casting. Serial casting can be used with kiddos who have various diagnoses, and has been proven effective in its ability to improve range of motion and quality of gait without interfering with their ability to perform daily activities. Serial casting is also a great alternative to surgery, and has improved results when followed by physical therapy and bracing.
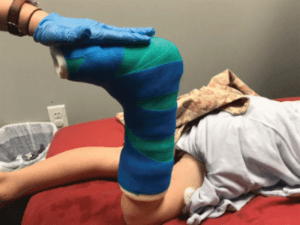
Typically, the parent and kiddo come back into the casting room with the trained therapist. To make it less scary, you are shown the different materials and tools used, and the kiddo can even pick out their own cast color (and sometimes more than one color). To make it more fun, kids typically choose to watch a movie or play a game while the therapist wraps their leg. It is important to know that the cast can come off if need be, however each cast lasts for 1 week. That means each week, the cast is removed, the therapist gives the muscle a little bit more of a stretch, and then new casts are made. This process continues until the full range of motion is achieved; typically, 4-6 sessions. They are given special “shoes” that strap onto the casts, and the therapist makes sure that they can safely walk with them on before leaving. Each week, the kids have fun decorating their casts and can continue with their daily lives as normal, just with 2 cool new accessories.
After the 4-6 sessions and the casts are removed for good, the therapist will assess the kiddo’s ability to walk, and may prescribe a few follow-up sessions to address their walking mechanics and/or strength. It is important to know that this muscle tightness could come back. Therefore, it is important to monitor the way your kiddo walks and does activities, and to continue with the home exercise program to ensure that all of the progress that has been made is maintained. It is also important to know that orthotics could be recommended after the course of casting; orthotics vary in size from shoe inserts to braces that go up the leg. The therapist will prescribe and fit the kiddo based on their individual needs. Overall, this process is to ensure the best results, meaning that it prevents injury and/or surgery, helps your child to walk efficiently with a normal pattern, and most importantly allows them to become a more functional and independent child.
For more information, please see our website at: www.abcpediatrictherapy.com
Resources
- Brouwer, B., Davidson, L. K., and Olney, S. J. Serial casting in idiopathic toe-walkers and children with spastic cerebral palsy. J Pediatr Orthop. 2000; 20(2): 221-5. http://www.ncbi.nlm.nih.gov/pubmed/10739286
- Fox, A., Deakin S., Pettigrew, G., Paton, R. Serial casting in the treatment of idiopathic toe-walkers and review of the literature. Acta Orthop Belg. 2006;72(6):722-730. https://www.ncbi.nlm.nih.gov/pubmed/17260610
- Glanzman, A., Flickinger, J., Dholakia, K, Bonnemann, C, Finkel, R. Serial casting for the management of ankle contracture in Duchenne muscular dystrophy. Pediatr Phys Ther. 2011; 23(3): 275-279. doi: 10.1097/PEP.0b013e318227c4e3.
4.Main, M., Mercuri, E., Haliloglu, G., Baker R, Kinali M, Muntoni, F. Serial casting of the ankles in Duchenne muscular dystrophy: Can it be an alternative to surgery? Neuromuscul Disord. 2007; 17(3): 227-230. https://www.ncbi.nlm.nih.gov/pubmed/17303425
- Pistilli, EE., Rice, T., Pergami, P., Mandich, MB. Non-invasive serial casting to treat idiopathic toe walking in an 18-month old child. NeuroRehabil. 2014; 34(2): 215-220. https://www.ncbi.nlm.nih.gov/pubmed/24419016.
- Novak, I., McIntyre, S., Morgan, C., Campbell, L., Dark, L., Morton, N., et al. A systematic review of interventions for children with cerebral palsy: A state of the evidence. Dev Med Child Neurol. 2013; 55(10): 885-910. https://www.ncbi.nlm.nih.gov/pubmed/23962350
- Barkocy, M., Dexter, J., Petranovich, C. Kinematic gait changes following serial casting and bracing to treat toe walking in a child with autism. Ped Phys Ther. 2017; 29(3): 270-274. doi: 10.1097/PEP.0000000000000404.
From time to time, you may see someone with a brace on and wonder what it is for. You may even see kiddos with braces on too. When you think of a brace, the first thing that probably comes to mind is: “they must have some sort of injury”. Although braces and splints are oftentimes related to injury, more often than not they are used to help provide support to an area of the body that has poor muscle function, low muscle tone, or just needs a little more than what their body as able to provide. It also may be that they help put that particular body part/region in a more appropriate alignment and/or may even be providing a low-load, long duration stretch to help manage things such as chronic muscle tightness, high muscle tone, or contractures. A contracture is defined as “a condition of shortening and hardening of muscles, tendons, or other tissue, often leading to deformity and rigidity of joint” (Oxford dictionary). This ultimately will improve their passive range of motion and allow a therapist to help the kiddo move through that new passive range and therefore improve strength and active range of motion needed for activities.
The most common brace or orthotic you will most likely see or encounter personally with yourself or child are those used for the foot, ankle or leg (aka lower extremity). Orthotics for the lower extremity range from shoe inserts to a small brace that stops just above the ankle to those that go higher up the leg. Starting at the least supportive orthotic, shoe inserts are typically used to help provide arch support and put the foot in optimal alignment to correct or prevent ailments such as pain in the foot, leg, or back as well as improve someone’s overall walking mechanics to prevent future injury. Next, there are the orthotics that go to the level of the ankle. These are called supramalleolar orthotics or SMO’s for short. These are common orthotics that can provide the alignment correction of a foot orthotic with additional support at the ankle. They are often used for kiddos who need a little more stability to either learn to walk or make walking more efficient and safer as well as for those who consistently toe walk, among other reasons. Finally, those braces that go up higher provide the same benefits as the SMO’s with even more support. These are typically recommended for those who have a more significant degree of deficits.
As a parent with a kiddo whose therapist recommends a splint, brace, or orthotic, it can be worrisome. You may be thinking that you don’t want your child to have to wear one or like the way they look. It is important to know that these supportive devices are only recommended when they are absolutely needed, and are prescribed in order to make your child more functional and independent now as well as make things easier for them in the future as they grow and get older. These devices will not only help them learn how to walk, but can help them with all activities of daily living as well as skills that are important for school and community-based activities, and later in life with driving and work skills.
If you have a little one and have noticed that they often fall, have an abnormal looking walk or run, or any of the above mentioned deficits, then a splint, brace, or orthotic may be helpful. To know whether or not something like this would help, contact a therapist for an evaluation. You can find more information on our website at: www.abcpediatrictherapy.com.
Hiking with the family is a great way to relax, exercise, play, learn, and explore new things. From a therapist perspective, this is also a low-stress and fun way to work on your child’s goals, no matter what the discipline. See below for ideas to enhance your hiking experience!
Physical Therapy
Climb, throw, and jump!
- Balance-Find trails that are uneven or not paved—a perfect opportunity to strengthen ankles, feet, toes and balance reactions!
- Strength- To get up and down those big hills we get use many different muscles. This challenges strength in our legs and our core.
- Natural Obstacle Course- Do you see that big log in the way or next to the path? Use it to balance, climb over, crawl under, or jump off!
- Body Awareness-Walking across the river on slippery rocks is a great way to address balance, body awareness, and motor planning. As always be very cautious around water.
- Throwing-Throwing rocks into the creek is a fun way to work on coordination for throwing. Make it a challenge to add in distance or aiming for an object.
- Jumping- Try jumping over or splashing in some puddles to build up that leg strength!
- There are so many ways to strengthen our bodies when playing outside!

Occupational Therapy
A multi-sensory experience!
- Sounds- Birds singing, trees creaking, or crickets chirping. The various frequencies that children hear allows for improved body orientation and spatial awareness!
- Sight and Smell- Search for flowers, rocks, animal tracks, and pine cones! These can also be great for crafting after the hike to target fine motor skills!
- Touch- Encourage kids to take their shoes off and feel the various textures on their feet—rocks, sand, water, mud or grass!
- Executive Functioning- Following a trail map targets directional skills for older kids.
- For the little explorers– Staying on the trail while scanning the woods is great for visual perceptual skills!
- Nature can be a great way for children to foster imagination and creativity!

Speech Therapy
Oh, the Things You Can Say!
Early Language/First Words: Keep words simple, “go,” “wet,” “up,” “in,” “splash,”
- Language Comprehension: Follow directions and teach spatial concepts such as “Walk through the tunnel,” “Go up the hill,” “Walk around the tree”
- Vocabulary and Describing: Work on new words and describing what you see, feel or hear. “The mud is sticky and slimy!”, “Can you find a bumpy rock? What else is bumpy?” “The water is cold,” “Do you see the bird way up high in the tree?” “The bridge is wiggling!!
- There is so much to talk about, learn and explore in nature!

Always remember general safety when going on a hike and ask your healthcare provider if you have any concerns. For more generalized tips and tricks for hiking with kids, check out the following resources. Happy hiking!
American Hiking Society https://americanhiking.org/resources/hiking-with-kids/
National Park Service https://www.nps.gov/subjects/trails/hiking-with-kids.htm
Hike it Baby https://hikeitbaby.com/blog/get-family-on-trail-with-proven-helpful-
For more information, visit https://www.abcpediatrictherapy.com/
Blog and pictures provided by: B. Kerbe Shephard, OTR/L, Michelle L. Huss, M.A. CCC-SLP, Rachel Menkedick, PT, DPT
 Skip to content
Skip to content